Endodontics
What Is Endodontics?
Endodontics is an area of dentistry that deals with the diagnosis and treatment of the dental pulp, which contains nerve fibers, tiny veins and arteries, lymph vessels and connective tissue deep inside your teeth.
What Is A Root Canal?
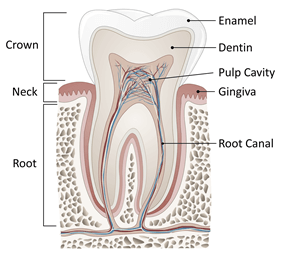
A root canal is actually a specific part of tooth anatomy.
Let’s take a quick look at tooth structure. The thin hard white surface that you brush everyday, is the enamel. Just underneath is a living calcified tissue called dentin. If you repeatedly brush your teeth very aggressively or your gums have receded, you may notice the dentin just below where the enamel ends at the gum line and your tooth root begins.
Dentin makes up the majority of your tooth’s structure and is typically a pale yellow color, but can range from gray to black. The dentin forms at least one, but usually not more than four roots, for each tooth.
Each tooth’s nerve and blood supply enters the tooth at the very tip of a root, runs through a “root canal” and into the pulp chamber. When a tooth becomes infected due to deep decay, fracture or injury, bacteria can seep into the pulp and it can die. Your body recognizes that dead pulp and tries to clean it up with increased blood flow and cellular activity in the area, also known as inflammation. This produces pressure that cannot be relieved from inside the tooth.
Pain inevitably follows, usually lots of it! It is at this point that root canal treatment is necessary to save the tooth. The only other option is extraction.
Why Do I Need Root Canal Therapy?
Infection is never a good thing to leave in the body. But, in this case, the simple answer to “why” is pain! Even though it seems to come and go, that only lasts for a short time. It will come back! When the pulp becomes infected, biting down, chewing and hot or cold food and drink will only make it more apparent that something needs to be done about it. Pain is present because an abscess usually forms and tries to expand with nowhere to go — that is why extractions work for abscesses — but then your tooth is gone. It will not heal itself, and, without treatment, the infection only spreads until the tooth falls or is taken out. Extraction may seem less expensive, but then the space created by the missing tooth brings other problems and expensive solutions. A better choice is to treat the pulp area at a 95% success rate and usually, in most cases, in a painless fashion.
What Is Involved In A Root Canal Procedure?
Root canal treatment is needed when the dental pulp (center of the tooth) dies or becomes infected. This can be after an injury, crack or, most often, from decay.
Once we agree to proceed with treatment, your tooth is numbed and an opening is created so we can clean out and kill the invading bacteria. The canal is cleaned of diseased nerve, tissue, etc. then, in our office, we introduce laser energy via a special radial laser tip into the canal in order to kill additional bacteria which may be hiding in the microscopic tubules of the dentin. It is an advanced procedure which can only help, not hurt, our goal of eliminating the infection completely and ultimately saving your tooth.
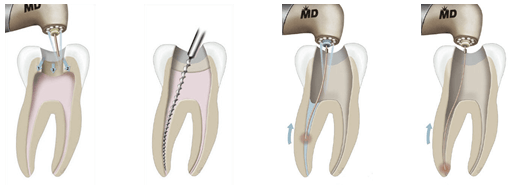
Depending upon the condition of your tooth, this procedure might require two visits and usually requires a crown to strengthen tooth structure or improve its appearance. It saves your tooth hopefully so you can chew with it for a lifetime.
We recently added high tech tools – Lasers and 3D digital x-ray – to make treatment even more predictable. Be assured, this is a very common procedure that we do almost daily in our dental office. And, like most problems in dentistry, early diagnosis and treatment make the whole thing go a lot easier, so DON’T WAIT to come in if you have tooth pain!
Why Do Some Dentists Say All Root Canal Treatment Is Bad?
It is true that some dentists (a tiny minority) feel there is ample evidence to banish the use of all root canal treatment. But recognizing that teeth, good chewing and diet are very important to health, we don’t share that extreme view. If health concerns outweigh the good that root canal treatment can do, certainly removing a severely or long-standing infected tooth is best. And with recent advances using lasers in root canals, and other improvements, hopefully the “hidden bacteria” in the dentin tubules can be killed more effectively and cleansed from the tooth, so that more teeth can be predictably saved without overall health concerns.
What Are the Benefits Of Root Canal Treatment?
What Does Root Canal Treatment Have To Do With Lasers?
FAQ about Root Canals
Are there any options to root canal treatment?
The only alternative to root canal treatment is to have the tooth extracted, but you really should consider the effects of a missing tooth on your bite and the gradual shifting of your adjacent teeth. Extracting the diseased tooth may be less expensive in the short run, but ultimately, a dental implant and/or bridge are much more costly.
What are the risks or complications of this treatment?
Root canal therapy has a greater than 95% success rate, but sometimes a procedure needs to be redone due to diseased canal offshoots that went unnoticed or untreated, both of which rarely occur. Occasionally, a root canal therapy will fail altogether, marked by a return of pain or inflammation. Also, we see evidence on x-rays when the body continues to “reject” a tooth.
What is the main cause of root canal treatment failure?
It is usually because there are tiny, unsealed, microscopic, branched canals that still hold bacteria and their toxins they produce. These microscopic canals are impossible to see and therefore treat to a good seal. This is hopefully where treatment with laser energy comes in. Although current research is incomplete in this area of study, it seems most reasonable that laser light will help and definitely not hurt.
